I read an enjoyable and thought provoking blog by Dave Leyland on the topic of Pelvic Alignment. The ever elusive human body fuels many opinions making this a good topic for discussion and thoughts.
With that said, here are mine.
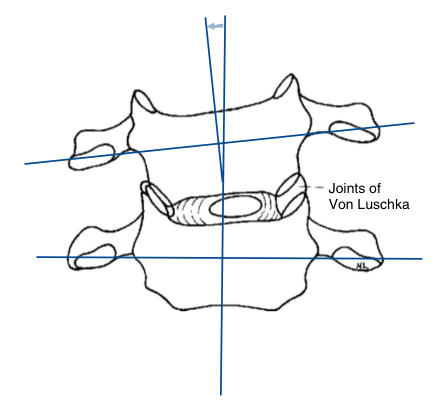
‘Alignment’ first reared its head in my early student days when reading some chiropractic content online. In addition, ‘subluxations’ in the spine were also mentioned and I thought this pushed quite a mechanical and fragile view of the body. After some investigation I found out the ‘spinal subluxation’ reference is not quite what it sounds, chiros are mostly relating to a movement restriction… so if a spinal segment is unable to extend upon its adjacent vertebrae, you would say it is flexed. If it was unable to rotate left you would say it is right rotated (even if its position is neutral, it is always in relation to the movement restriction), and this is said to be possible for any vertebral movement variation.
With regards to the pelvis, I would say there also can exist some movement restrictions/preferences which could explain small asymmetries in alignment, I would agree with Dave and put this down to the usage of muscles attaching to the pelvis (which could be an important finding).
However, we know symmetry is a rarity in function (eg right side dominance), so why are we/patients so keen to gain it in structure? The question I would like to push forward is, in palpatory assessment – are we really feeling pelvic bone movement/position?
Lets take these 2 examples:
Pubic tubercle level – hypertonia in the rectus abdominis on one side can raise tissues in this area assymetrically… is one bony tubercle either side of the symphysis really higher? Or are we feeling soft tissue tension?
The SIJ – this has been found to move a few degrees on average (depending on what article you read), but in say the stork test, we need to ask are we really feeling the PSIS and sacral bone move, or are our hands moving with the superficial tissues? … more importantly, is this tissue movement clinically relevant?
My opinion is yes, and here is why.
The relevance of a hypertonic ipsilateral rec. abdominis depends on the skill set of the practitioner interpreting the collective assessment. But if we are ‘treating what we find’, I think it can and should be treated, especially if that patient is complaining of pubic symphyseal pain (screening of adductors also needed).
More interesting is the stork test result, as we all know, the SIJ has no monoarticular muscles, but does have fascia and other connective tissue traversing it. The importance and understanding of fascia dynamics is growing in the industry, and in this example of a clinical test, I think the movement felt is soft tissue/fascia more than the joint.
Why is this important? Well these tissues are going to move according to underlying osseous structures, also according to muscular involvement – controlling the global connective issue drag. Is it the contralateral lumbar mulifidus and musculature which help pull and stabilise in this test? Is it a lack of their involvement which leads to a positive finding? I am yet to read an explanation/ theory other than SIJ movement. I will say however that if SIJ movement is the sole explanation – the tissue movement in most cases would indicate more than a few degrees! Which is why I believe otherwise.
So there is a piece of my mind on the topic, I am keen to hear others thoughts and opinions on this.
NOTE: If you are keen to read more on the pelvis, I recommend literature by physiotherapist Diane Lee who specialises in this area, and incidentally regards the stork test as clinically relevant for SIJ involvement (link).